Managing the growing cost of wildfire
Key Takeaways
- Wildfire smoke is rapidly becoming a regional air pollution issue similar to acid rain and ozone in the 1980s, threatening decades of air quality improvement. Regions in the West are being hit hardest, with massive health impacts.
- More investment in fire management — including controlled burns — is the best way to quickly reduce public health risks from wildfire.
- Current policies make it difficult for state and federal authorities to use those methods.
- If global greenhouse gas emissions are not brought under control, fire seasons will grow longer and more damaging, even with better management strategies.
The American West is experiencing unprecedented wildfire activity. Five out of the six largest fires on record in California are still burning, and the state has witnessed more charred acreage than any year in recorded history. Oregon and Washington have also suffered multiple catastrophic wildfires this year. Across the U.S. as a whole, the average annual acreage burned by wildfires doubled over the last two decades. And this year’s fire season is far from over.
News coverage and government intervention understandably focus on the immediate consequences of these fires: protecting homes and lives directly in the path of the flames and reporting on those homes and lives that were lost. But the negative consequences of the dramatic increase in wildfire activity extend far beyond these immediate impacts, in ways that will increasingly touch the lives of most Americans.
Smoke from wildfires is rapidly worsening air quality across much of the country, with demonstrable health consequences that affect people no matter where they live or how much money they have.
These problems shouldn’t come as a surprise. They are the result of our own actions and policy choices, both in how we manage forests and how we manage the climate. Without significant changes to those actions and decisions, we may look back on the 2020 fire season as one of the least destructive of the 21st century rather than as one of the worst in our history.
In this policy brief we review recent trends in wildfire activity, quantify how the smoke from these wildfires is affecting air quality and health across the U.S., and discuss what policymakers can do to help reduce wildfire risk. Our work builds in part on a recent NBER study we and colleagues released. [1]
Wildfires are reversing air quality gains
Figure 1 shows the number of acres burned by wildfires has roughly doubled since 2000. These increases have been driven by the combination of a warming climate, which has killed hundreds of millions of trees in Western forests and made a tinderbox out of others, and — somewhat ironically — by a legacy of quickly putting out all fires, which has left massive amounts of unburned fuel ready to ignite.
Where there’s fire, there’s smoke. The rapid increase in wildfire activity has led to a naturally expected increase in wildfire smoke, both in the regions where the fires occur as well as thousands of miles away (e.g., the U.S. East Coast) where large wildfires rarely occur but where smoke from distant fires is blown.
Recent satellite-based estimates of the location of wildfire smoke plumes show a steady increase in “smoke days” across the U.S. — days when a smoke plume is overhead. While the Western U.S. experiences more of these smoke days on average, clear positive trends in smoke days are apparent throughout the country (see Figure 1b). Smoke is fast becoming a regional air pollution issue similar to acid rain and ozone in the 1980s, with implications for both source and downwind states.
This increase in smoke threatens to undermine decades of air quality improvements across the country — improvements driven largely by federal policies (specifically the Clean Air Act), which have led to substantial health benefits for millions of Americans.[2] Key pollutants such as PM2.5 had been trending steadily downward across most of the U.S. until the last few years, at which point progress flattened and — in parts of the West — started to reverse (Figure 1c).
Our research estimates that as recently as 15 years ago, wildfires were responsible for roughly 5 to 10 percent of total PM2.5. Today we estimate that wildfires represent about 25 percent of PM2.5 across the U.S. and sometimes more than 50 percent throughout much of the West. Increases in wildfire activity are indeed a primary force in worsening air quality throughout much of the country.
The health costs of wildfire smoke are massive — and growing
Most people have an intuitive sense that breathing wildfire smoke — or any sort of air pollution — is likely not good for them. There is a growing body of scientific evidence that puts numbers on this intuition, and the numbers are quite high. Studies clearly demonstrate that breathing PM2.5 from wildfire smoke or other sources leads to a vast array of negative health and economic impacts, from reduced respiratory and cardiovascular function to declining cognitive and labor output to — in the worst cases — early death.
To illustrate how bad acute wildfire smoke events can be for health, we study the 2020 wildfires in August and September across the West Coast, which blanketed most of the region’s 50 million residents with dense smoke for weeks.
Figure 1. Trends in wildfire and its consequences.
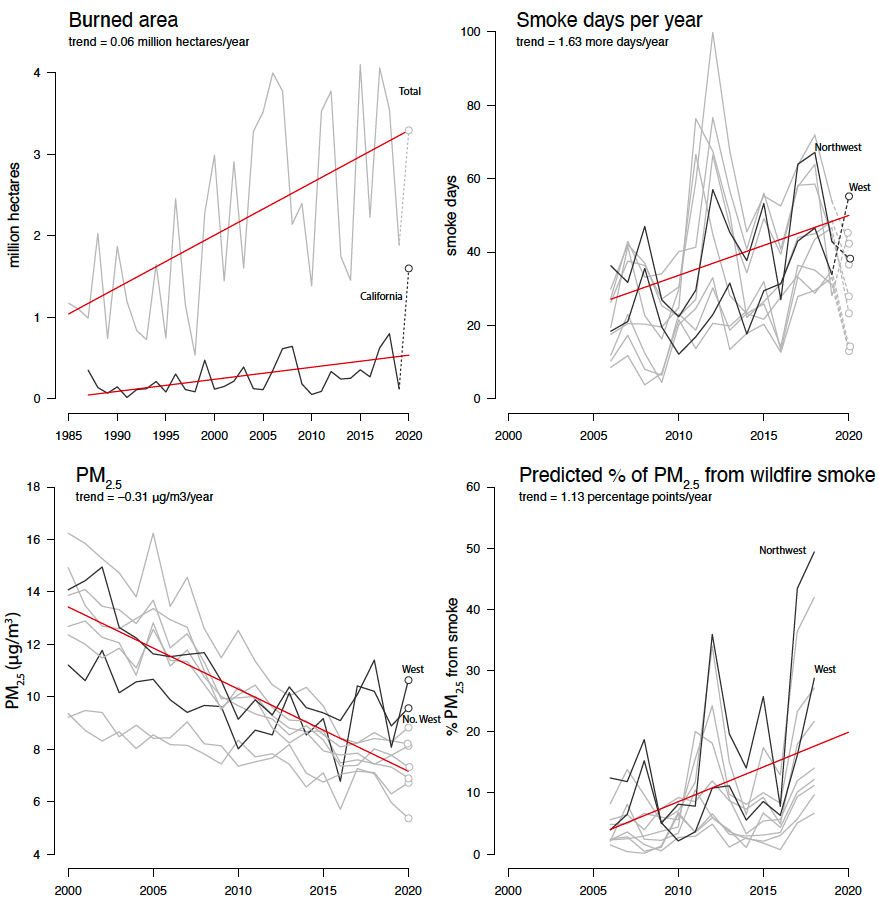
Data sources
- Panel a Burned Area: National Interagency Coordination Center (NICC), Wildland fire statistics (2019)
- Panel b Smoke days per year: NOAA Hazard Mapping System Fire and Smoke Product
- Panel c PM2.5: EPA
- Panel d predicted % of PM2.5 from wildfire smoke: Marshall Burke, Anne Driscoll, Jenny Xue, Sam Heft-Neal, Jennifer Burney, and Michael Wara. “The changing risk and burden of wildfire in the US”, NBER Working Paper 27423, 2020.
Figure 2 shows how daily levels of PM2.5 during these two months deviated from recent historical daily averages across major West Coast population centers. Areas such as the San Francisco Bay Area, Portland, and Seattle — which typically enjoy PM2.5 levels below 10 micrograms per cubic meter — had readings in the 100s to 300s for weeks, making them the most polluted cities on the planet at the time.
To calculate likely health costs of this exposure, we combined observed pollution levels with recent high-quality estimates[3] from Medicare data of how changes in daily pollution have historically affected the health of the elderly in the U.S. This gives us an early estimate, based on the best possible science, of how ongoing fires are affecting population health.
These estimates suggest that for every one microgram increase in PM2.5 on a given day, mortality over the next few days rises by about one person per million individuals. When combined with the increases in PM2.5 shown in Figure 2, the implied excess death totals are staggering: Hundreds of elderly individuals likely died from smoke exposure in each major West Coast population center and thousands likely died across California alone (see right axis, Figure 2).[4]
These can be considered “excess” deaths — deaths that would not have occurred in the near term were it not for the smoke exposure, and they far exceed (by one to two orders of magnitude) those who died in the wildfires. We emphasize that these numbers are estimates of the likely number of lives lost, based on the best data we have at hand; a full accounting will take years and would include not just seniors but the entire population.
These estimates comport with other ways of calculating the health and mortality costs of wildfires. Our findings estimate that wildfire smoke is likely responsible for 5,000 to 15,000 deaths in an average year in the U.S. Smokier years like 2018 or 2020 will have a much higher death toll.
Figure 2: Wildfires on the West Coast.
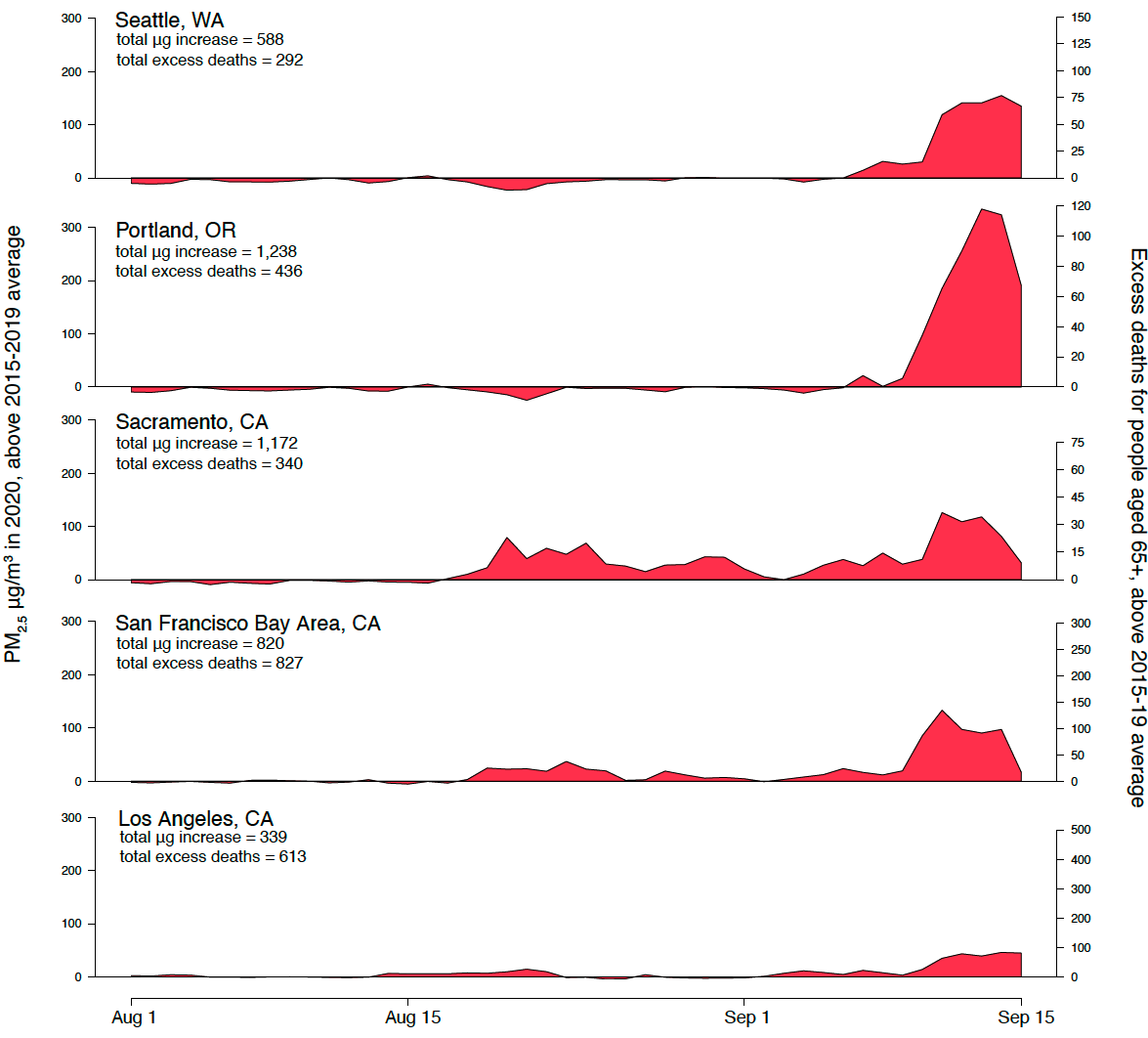
Data Sources
- PM2.5 data comes from the EPA’s AQS database
- Estimated relationship between PM2.5 and mortality used for the excess mortality calculations comes from Deryugina et al 2019. “The mortality and medical costs of air pollution: Evidence from changes in wind direction”. American Economic Review, 2019
- Population data used for the excess mortality calculations come from the American Community Survey
Federal policy must be prompt
What should be done about these rapidly growing health costs of wildfire smoke exposure? Wildfire is not a problem that can simply be left to state and local governments (although they have a role to play as well). This is because, as shown in Figure 3, about 60 percent of the burned area from wildfires is on federal land. A coordinated federal-state policy response will be a key part of the solution.
One complicating factor in mounting a coherent response is that legislation that empowers air regulators to control pollution — the Clean Air Act and its multiple revisions — is currently ill suited to address pollution from fires.
Wildfire smoke is considered an “exceptional” emission source under the Clean Air Act, not subject to human control and thus not counted toward attainment of national health-based standards for air quality. But while one of the main interventions for fighting fire — the use of prescribed burns — is under human control, the emissions from those intentionally set fires are regulated by and subject to burdensome environmental permitting.
This, along with liability issues, has contributed to the underutilization of prescribed fire as a risk-reduction tool. Outside the Southeastern U.S., the number of acres on which prescribed burns occur is a tiny fraction of the number of acres on which wildfires occur (see Figure 3).
Obviously, a wildfire cannot be regulated in the same way as a smokestack or a tailpipe. But current policies have created an unacceptable irony: Deciding against controlled burns and thereby increasing wildfire risks faces no penalty. But reducing those risks by doing a controlled burn can incur significant regulatory costs. This clearly cannot be the way forward.
Now and later: What policymakers can do
Evidence suggests that dramatically expanding “fuels management” strategies, including use of prescribed fire, is the best way to quickly reduce public health risks from wildfire. This has been common knowledge in the land management community since at least the 1980s.
But the agencies and land managers charged with implementing this process face the challenge of ever-escalating fire suppression costs, the regulatory barriers to greater use of fuel management tools, and institutional incentives within fire and land management agencies that promote fire suppression (i.e., extinguishing wildfires) and disaster response over prescribed burns and risk reduction.
In addition, there is the question of where to find the resources to engage in fuels management at a scale large enough to matter. Estimates of the cost of prescribed fire range between $100 and $1,000 per acre of treated forest. And in California alone, there are somewhere between 10 and 30 million acres that would benefit from fuel reduction treatment.
In the long run, if global greenhouse gas emissions are not brought under control, fire seasons will grow longer and more violent, even with better fuels management. So we must reduce the impacts on climate that are also an important underlying driver of intensifying wildfires in California and the West.
Important next steps are to further evaluate the health and economic impacts of smoke and the potential impacts from a dramatic scale-up in prescribed fire. Prescribed fire remains the least expensive approach to treating the millions of acres that are at risk, but will also produce smoke impacts.
We should be willing to tolerate some degree of smoke impacts from prescribed fire in order to reduce risks of much more harmful catastrophic fires. But this risk balancing will require careful analysis and targeting of fuels treatments with downwind public health impacts of the smoke from both controlled and uncontrolled fire in mind. Air regulators should be empowered to conduct this analysis, funding at a scale sufficient to actually reduce risk needs to be found, and the regulatory balance between the intentional decision to burn and not to burn needs to be corrected.
If we fail to do this, the fire season we are experiencing in 2020 will pale in comparison with what awaits in the years ahead.
Figure 3. Average wildfire and prescribed burned area over the past 20 years by jurisdiction and region.
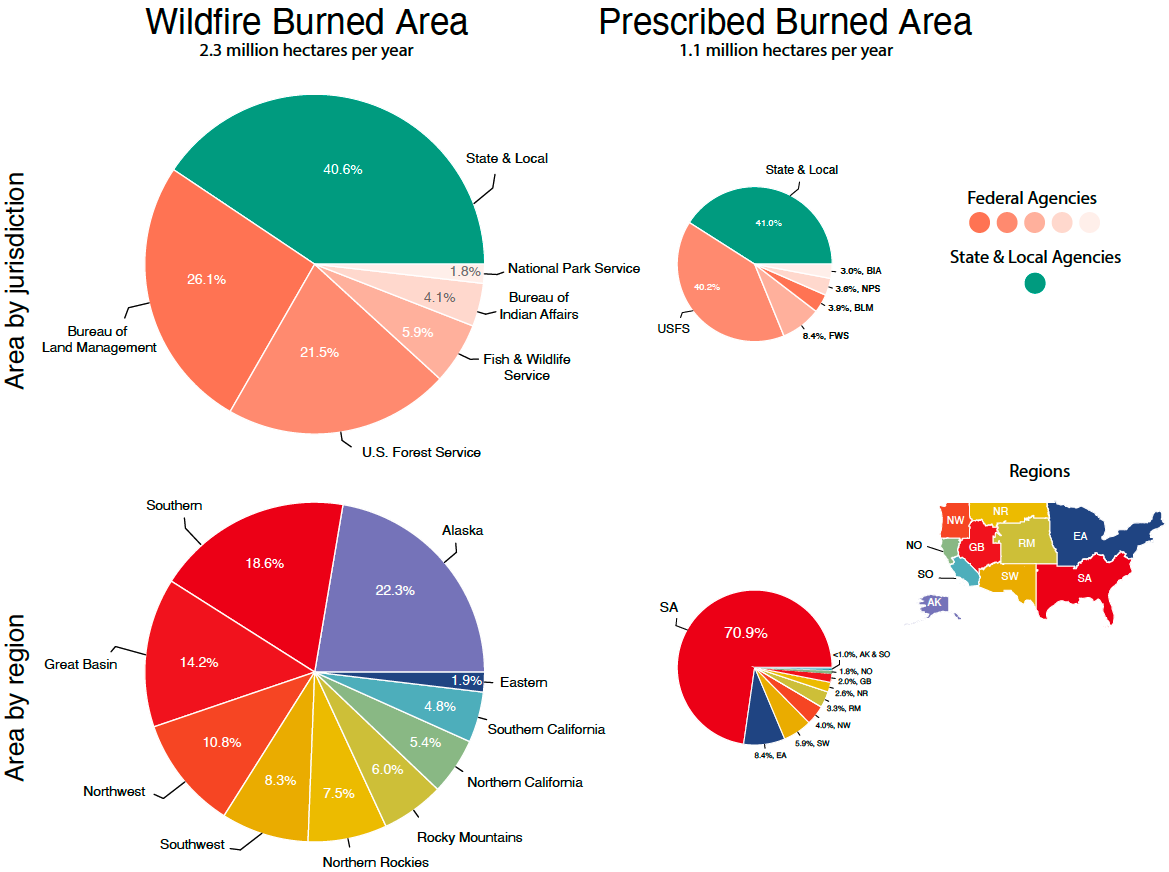
Data Source
Footnotes
1 Marshall Burke, Anne Driscoll, Jenny Xue, Sam Heft-Neal, Jennifer Burney, and Michael Wara. “The changing risk and burden of wildfire in the U.S.” NBER Working Paper 27423, 2020.
2 See EPA “The Benefits and Costs of the Clean Air Act,” March 2011; Janet Currie and Reed Walker, “What Do Economists Have to Say About the Clean Air Act 50 Years After the Establishment of the Environmental Protection Agency?” Journal of Economic Perspectives, 2020.
3 Deryugina et al. 2019. “The mortality and medical costs of air pollution: Evidence from changes in wind direction.” American Economic Review, 2019.
4 See Marshall Burke and Sam Heft-Neal, “Indirect mortality from recent wildfires in CA” for additional detail on this calculation.